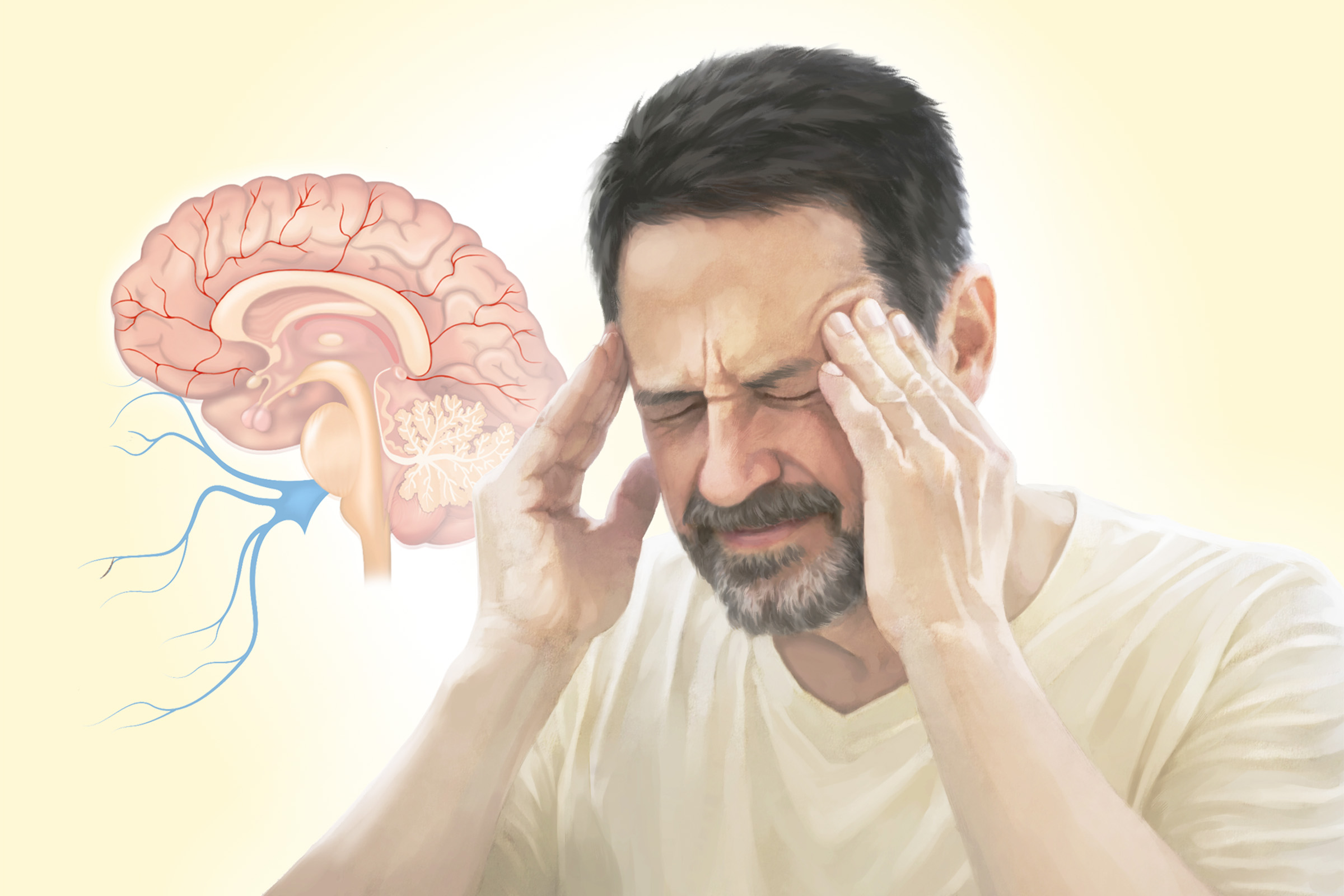
Phases of Migraine
Most migraine attacks unfold in stages, and recognizing them can help people act early to reduce severity. Not everyone experiences every phase, and phases can overlap.
- Visual disturbances (scintillating scotoma): A brief blind spot in the center of vision followed by shimmering, brightly colored, zig-zagging lights
- Numbness or tingling: “Pins-and-needles” sensations in the arm, leg, or face
- Muscle weakness: Often affecting one side of the body
- Difficulty speaking: Trouble forming or finding words
- Unusual sensory experiences: Hearing strange sounds or music
- Involuntary movements: Such as jerking motions
- Throbbing or pulsating headache: Typically builds gradually and intensifies over time
- Nausea or vomiting
- Sensitivity to light, sound, smell, or touch
3. Attack (4 to 72 hours): The migraine is in its active phase. A migraine headache usually begins gradually and intensifies over time. Pain is typically throbbing or pulsating and may be accompanied by nausea, vomiting, or sensitivity to light, sound, smell, or touch.
- Throbbing or pulsating head pain
- Nausea
- Vomiting
- Sensitivity to light, sound, smells, and touch
4. Postdrome (up to two days after): The postdrome phase can leave a person feeling drained, confused, and washed out. Some may experience mood changes or brief pain triggered by sudden head movements, while others even feel unusual elation. Concentration may be difficult, dizziness can occur, and overall energy is typically low.
5. Interictal (between attacks): The period between migraine attacks with an unpredictable duration, which may leave people anxious about when the next episode might strike.
Different Types of Migraine
Different types of migraine also have varying symptoms.
Emergency Symptoms
Most migraines, while debilitating, are not medically dangerous. However, seek immediate medical care if you experience a sudden, severe “thunderclap” headache that reaches maximum intensity within seconds, or a headache that is different from your usual pattern.
- Calcitonin gene-related peptide (CGRP): Causes blood vessels to dilate and activates pain-sensitive nerves, contributing to pain and light sensitivity.
- Serotonin: Influences blood vessel swelling, head pain, sleep, mood, and cognitive changes.
- Dopamine: Affects mood, motivation, focus, and sleep, and is strongly linked to nausea, yawning, dizziness, and vomiting—common migraine symptoms.
In people who experience aura, researchers believe the symptoms result from a phenomenon called cortical spreading depression—a slow wave of electrical activity that moves across the brain, temporarily disrupting specific regions. When it passes through the visual cortex, for example, it can cause the characteristic shimmering lights or blind spots of visual aura.
- Genetics and family history: Migraine has a strong genetic component, with close relatives of affected individuals having about three times the risk. It is likely influenced by multiple genes interacting with environmental factors, particularly genes involved in nerve and blood vessel function.
- Sex and hormones: Migraine is significantly more common in women than in men, affecting approximately 17 to 19 percent of women compared with 5 to 7 percent of men, according to a 2024 systematic review. Hormonal fluctuations during the menstrual cycle and pregnancy likely contribute to the higher rates of migraine in women.
- Co-existing medical conditions: Depression, anxiety, fibromyalgia, sleep apnea, and postural orthostatic tachycardia syndrome (PoTS) can increase migraine risk. Effectively managing these conditions may improve migraine treatment outcomes.
- Obesity: In addition to being a risk factor, obesity worsens migraine by increasing headache frequency in people with episodic migraine and raising the risk of progression to chronic migraine.
- Childhood trauma and abuse: Physical, emotional, and sexual abuse in childhood can alter neurological development in ways that increase the risk of migraine and other pain conditions. Emotional abuse appears to have the strongest association.
- Ethnicity: Migraine is more common among Native Americans than other ethnicities.
Migraine Triggers
- Stress and emotional factors (most common—up to 80 percent of cases): Examples include stress, anxiety, tension, depression, and even excitement.
- Physical triggers: Examples may include fatigue, sleep loss or irregular sleep patterns, intense physical exertion, neck or shoulder tension, eye strain (such as prolonged computer use), and dental issues like teeth grinding.
- Skipped meals and dietary factors (around 57 percent of cases): Skipping meals, irregular eating, dehydration, and specific foods or additives are commonly reported. Alcohol—particularly red wine—is the most frequently cited food-related trigger. Other common offenders include chocolate, aged cheese, citrus fruits, caffeine, MSG, tyramine, aspartame, and nitrates. Emerging evidence suggests that some food cravings may actually be early prodrome symptoms rather than triggers.
- Weather and environmental changes (around 53 percent of cases): Shifts in humidity, barometric pressure, or temperature are frequently reported triggers, as are bright or flickering lights, loud noises, strong odors, and smoky or stuffy environments.
- Certain medications: Some sleeping tablets, the combined oral contraceptive pill, other estrogen-containing contraceptives (such as the ring or patch), and hormone replacement therapy.
- Illnesses: Infections like the common cold or influenza can trigger migraines, especially in children.
- Blood tests: Check for medical conditions through various lab analyses.
- Sinus X-rays: Detect congestion or other sinus issues that may contribute to headaches.
- MRI: Uses magnets and radio waves to create detailed images of organs and structures.
- CT scan: Combines X-rays and computer technology to produce detailed images of the head or body, showing more detail than standard X-rays.
- Spinal tap (lumbar puncture): Measures pressure in the spinal canal and allows testing of cerebrospinal fluid to detect infections or other problems.
- Electroencephalogram (EEG): Evaluates for possible seizures.
- Headache diaries: Used in migraine diagnosis to track the frequency, duration, triggers, and characteristics of headaches, helping clinicians identify patterns and confirm a migraine diagnosis.
Acute/Abortive Treatments
These medications can stop a migraine at its onset or prevent it from worsening once it begins.
Treatments to Reduce Migraine Frequency
Migraine treatment helps reduce the frequency, severity, and duration of attacks, improves response to acute medications, and lowers disability. It can also decrease the need for pain relievers, helping prevent medication overuse headaches. It is typically considered when migraines are frequent (more than four per month), severely disabling, or not well controlled with acute medications alone.
Neuromodulation Devices
Wearable or handheld devices that stimulate specific nerves in the body offer a nondrug option for both treating migraines and preventing attacks. They are well-tolerated with few side effects.
- External trigeminal nerve stimulation (eTNS) device: Used for both acute and preventive treatment of episodic migraine in adults, it is worn on the forehead. It works by stimulating the trigeminal nerve, which is involved in migraine.
- Remote electrical neuromodulation (REN) device: It is worn on the upper arm for episodic and chronic migraine in adults and adolescents. It activates the body’s natural pain-inhibition system to reduce migraine pain.
- Vagus nerve stimulator: This noninvasive handheld device is applied to the neck and is used for both acute and preventive treatment of migraine and cluster headaches in adults and adolescents.
- Single-pulse transcranial magnetic stimulation device: Worn or held against the back of the head, it delivers brief magnetic pulses to the skull to interrupt abnormal activity associated with migraine. Used for both acute and preventive treatment.
Alternative/Complementary Therapies
- Acupuncture: A 2025 meta‑analysis found acupuncture significantly reduced migraine frequency, duration, and headache days compared with control treatments, with few side effects. It is a well-supported complementary option.
- Craniosacral therapy: A gentle, noninvasive manual therapy combining massage and osteopathic techniques. A 2022 study found it may help reduce migraine pain and frequency and decrease disability and medication use.
- Feverfew: A traditional herbal remedy for migraine. A 2025 meta-analysis found it reduced migraine attack frequency and duration, although it did not significantly improve nausea or other associated symptoms.
- Green light therapy: A 2025 study found that regular exposure to green light reduced migraine pain intensity and frequency, improved quality of life, and decreased medication use.
- Wuzhuyu decoction (traditional Chinese Evodia rutaecarpa medicine): A 2018 study found this herbal formula reduced migraine pain intensity and frequency, and decreased pain medication use, more quickly than a placebo.
- Goreinsan (traditional Japanese medicine): A 2018 study of 45 patients found this ancient formula improved headache intensity and frequency, particularly for weather-related migraines.
Novel and Emerging Therapies
The following treatments are investigational or newly available and may not yet be widely accessible.
- CT-132: This is the first FDA-approved prescription digital therapeutic, which is software-based medical intervention, for preventing episodic migraine. Delivered through a smartphone app and used alongside existing treatments, it was approved based on two randomized clinical trials showing significant reductions in monthly migraine days.
- Migraine Therapy System: A pilot study showed that this new fully implantable Migraine Therapy System led to lasting reductions in headache frequency and severity in people with chronic migraine.
- PACAP-targeting monoclonal antibody: A promising new treatment for patients who do not respond to CGRP-based therapies. Pituitary adenylate cyclase-activating polypeptide (PACAP) appears to trigger migraines through a distinct pathway, making it an alternative target for future drugs.
Diet
A 2021 study found that a 16-week diet high in fatty fish helped 182 adults with frequent migraines reduce both the frequency and intensity of their migraine headaches. More broadly, it’s generally better to eat more protein, limit simple carbs and processed foods, and have three regular meals daily without skipping.
Supplements
The following supplements are frequently discussed for managing migraine.
- Magnesium: A 2024 meta-analysis found that magnesium supplementation significantly lowered migraine frequency and severity, and the number of headache days each month. Magnesium oxide is a commonly used form of magnesium to help prevent migraines.
- Coenzyme Q10 (CoQ10): Coenzyme Q10 is a fat-soluble compound made by the body and obtained from food that helps produce cellular energy (ATP) in mitochondria and also acts as an antioxidant. A 2025 meta-analysis found that CoQ10, either alone or combined with other supplements, helped reduce migraine frequency, severity, and duration.
- Riboflavin (vitamin B2): A 2025 review found that in one clinical trial, adults who took 400 mg of riboflavin daily for three months had about 50 percent fewer migraines and 40 percent fewer headache days compared with placebo, thus supporting its use for migraine prevention.
Aromatherapy
Essential oils can help with migraine pain and other symptoms such as nausea, relaxation, sleep, and easing muscle tension. However, use caution if strong scents trigger your symptoms. The most commonly used oils are:
- Lavender: In a 2012 study, 47 adults with migraines inhaled lavender essential oil for 15 minutes during an acute attack and experienced a significantly greater reduction in headache severity over two hours compared with a group that didn’t use lavender oil. In a 2016 study, lavender essential oil used alongside standard migraine prevention therapy reduced migraine frequency and severity, suggesting potential preventive benefits.
- Peppermint: A 2019 study found nasal application of peppermint oil significantly reduced headache intensity and frequency, relieving pain in most patients with migraine. Its effectiveness is similar to lidocaine, a type of anesthetics.
Meditation
A 2017 study involving more than 40 patients with chronic migraines found that mindfulness-based training produced results similar to conventional therapy. Both groups experienced reductions of six to eight headache days per month, used about seven fewer medications per month, and showed improved disability scores. Around half of the patients in each group achieved an over 50 percent reduction in headaches, and most no longer met criteria for chronic migraine.
Other Lifestyle Modifications
Please consult your doctor for suggestions to your specific situation.
- Sleep: A 2022 study found that people who experience frequent migraines often have poor sleep quality. Aim for 7 to 8 hours nightly, keeping a consistent sleep schedule and avoiding naps. If you can’t sleep after 20 to 30 minutes, get up and try relaxation techniques.
- Exercise: Start gently and exercise when migraine-free, aiming for approximately 30 minutes, three times a week. Moderate activity like walking is best; intense exercise can trigger migraines.
- Hydration: Drink 7 to 8 glasses of water daily and limit caffeine.
- Follow a consistent daily routine: regular sleep, meals, hydration, and exercise reduce vulnerability to triggers.
- Identify and avoid modifiable triggers using a headache diary.
- Consider preventive medication if attacks are frequent or disabling (see the treatment section above).
- Practice regular stress reduction through yoga, meditation, cognitive behavioral therapy, or other techniques.
- Maintain a healthy weight, as obesity worsens migraine frequency and is a risk factor for progression to chronic migraine.
- Manage co-existing conditions such as depression, anxiety, and sleep disorders, which can amplify migraine burden.
- Mental health issues: People with migraine may have a slightly higher risk of mental health conditions, including depression, bipolar disorder, anxiety, and panic disorder.
- Medication-overuse headaches: These are caused by taking too much headache or pain medicine. People with migraines may try to relieve their pain by using these medications frequently, but over time, this can actually make headaches happen more often. This creates a cycle where the medicine meant to help becomes the cause of new headaches.
- Ischemic stroke: This occurs when a blood clot blocks blood flow to the brain. People with migraine with aura have about twice the risk of ischemic stroke compared to those without migraine, although the overall risk remains low.
- Status migrainosus: In this rare but serious complication, severe pain and nausea last longer than 72 hours. The symptoms can be so intense that hospitalization may be required.
- Persistent aura without infarction: Aura symptoms last more than one week, but brain imaging shows no evidence of stroke.
- Migrainous infarction: One or more aura symptoms occur along with reduced blood flow to the brain during a typical migraine attack.
- Migraine aura-triggered seizure: A seizure is triggered during a migraine attack that includes aura.
- Immobility: Severe pain during attacks can prevent normal function. Chronic migraine in particular can cause significant daily impairment and loss of productivity.