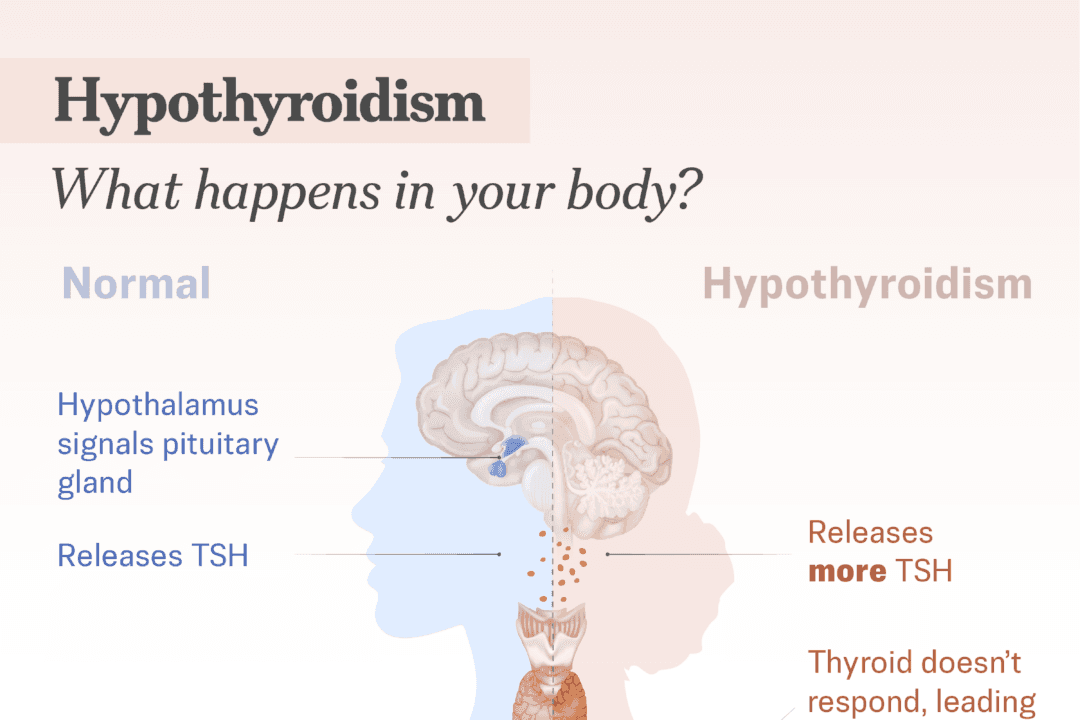
Feeling tired, lacking energy, and persistently in a low mood—these can all be signs of hypothyroidism, or an underactive thyroid. Hypothyroidism is the most common thyroid disorder in the United States, affecting about 5 in 100 Americans age 12 and older.
Although hypothyroidism is not typically curable, most cases are mild, cause few noticeable symptoms, and can be effectively managed.
Early Signs of Primary Hypothyroidism
Initial symptoms may include:
- Persistent Fatigue or Slowed Thinking: Low thyroid function reduces energy levels and slows physical and mental activity.
- Constipation: Slowed digestive muscle activity leads to fewer bowel movements.
- Increased Sensitivity to Cold: Reduced cellular activity lowers heat production, causing people to feel cold even when others are comfortable.
- Joints and Muscle Aches: Slowed metabolism in muscle and connective tissue can cause weakness and cramps.
- Pale or Dry Skin: Reduced oil production and slower skin cell turnover can make skin dry and flaky.
- Low Mood or Depression: Impaired brain energy metabolism may lead to trouble concentrating, memory lapses, and decreased interest in usual activities.
- Thinning Hair and Brittle Nails: Reduced nutrient and oxygen delivery to hair follicles and nail beds can weaken growth.
- Weight Gain: Fewer calories are burned for energy, increasing fat storage even if appetite declines.
- Heavy or Irregular Menstrual Cycles: Disrupted hormone balance can make menstrual periods heavier, more frequent, or stop entirely.
Later-Developing Symptoms
If untreated, primary hypothyroidism may lead to:
- Reduced Taste and Smell: Slowed metabolism can impair sensory perception.
- Hoarse Voice: Swelling of the vocal cords or acid reflux related to slower digestion may alter the voice.
- Swelling of the Face, Hands, and Feet: Fluid retention can cause puffiness and bloating.
- High Cholesterol Levels: Low thyroid hormones can raise total and low-density lipoprotein “bad” cholesterol levels.
- Slowed Speech: Overall slowing of the nervous system may affect speech patterns.
- Thinning of Scalp and Outer Eyebrow Hair: Though uncommon, hair loss may occur because thyroid hormones support follicle function.
- Slowed Heart Rate: Reduced thyroid hormone levels can weaken heart function and, in severe cases, increase the risk of heart failure, particularly in older women.
Symptoms in Children and Adolescents
Symptoms may differ from those in adults, and some children have no noticeable signs.
- Newborns: Jaundice (yellowing of the skin and eyes), a hoarse cry, poor feeding, umbilical hernia (a protruding navel), constipation, and slow growth.
- Children: Slow growth, delayed tooth development, fatigue, an enlarged thyroid gland (goiter), and constipation.
- Adolescents: Delayed puberty, irregular or heavy menstrual periods, dry skin, slow heart rate, brittle hair or hair loss, and weight gain.
Symptoms in Older Adults
Symptoms in older people are often subtle or uncommon. Instead of classic signs, they may experience weight loss, confusion, reduced appetite, joint or muscle pain, weakness, or frequent falls. Because these symptoms overlap with normal aging, hypothyroidism is often overlooked. Although some experts suggest routine screening after age 70, most medical organizations do not recommend screening without symptoms to avoid unnecessary treatment.
Emergency Symptoms
Severe hypothyroidism, known as myxedema crisis, is a medical emergency requiring immediate treatment. Symptoms may include loss of consciousness, low blood pressure, low blood sugar, low body temperature, slowed breathing, or sudden changes in mood or behavior.
- Hashimoto’s Thyroiditis: A chronic autoimmune disorder in which the immune system mistakenly attacks thyroid tissue, causing inflammation and gradual loss of function. The gland may enlarge early in the disease and later shrink and scar. Hashimoto’s thyroiditis runs in families and is four to 10 times more common in women. It is also associated with other autoimmune conditions, including Type 1 diabetes, Addison’s disease, and rheumatoid arthritis.
- Previous Hyperthyroidism Treatment: Radioactive iodine therapy or surgical removal of the thyroid often results in permanent hypothyroidism. External radiation therapy to the neck or head may also impair thyroid function. In rare cases, damage to the pituitary gland disrupts hormone regulation.
- Certain Medications: Overtreatment with antithyroid medications such as propylthiouracil, methimazole, or iodide can cause temporary hypothyroidism. Other medications that interfere with thyroid function include lithium, iodine-containing heart medications such as amiodarone, interferon-alfa, and certain cancer therapies, including immune checkpoint inhibitors and tyrosine kinase inhibitors.
- Thyroiditis: Inflammation of the thyroid can cause stored hormone to leak into the bloodstream, temporarily raising hormone levels, causing thyrotoxicosis—a state of excessive thyroid hormone lasting for several months. Long-term damage may result in permanent hypothyroidism.
- Nutrient Deficiencies: The body needs about 150 micrograms of dietary iodine daily to produce adequate levels of thyroid hormones. Deficiencies in iodine, magnesium, vitamin B12, or vitamin D have been linked to impaired thyroid function.
- Congenital Hypothyroidism: Occurs when the thyroid gland does not develop or function properly before birth and affects about one in 2,000 to 4,000 newborns. Most cases happen spontaneously, although 10 percent to 20 percent are inherited. Because untreated cases can lead to intellectual disability and poor growth, newborns in the United States are routinely screened.
Subclinical hypothyroidism is an earlier, milder form defined by elevated TSH with normal T4 levels and few or no symptoms. It affects about 15 percent of older women and 10 percent of older men, particularly those with underlying Hashimoto’s thyroiditis. Patients who test positive for thyroid peroxidase antibodies are at higher risk of progressing to overt hypothyroidism, with research showing that approximately 50 percent may develop primary hypothyroidism within 20 years.
Risk Factors
Most risk factors for hypothyroidism are not modifiable, but awareness can help with early detection.
- Female Sex: Women are at higher risk than men.
- Older Age: Risk increases after age 60.
- History of Thyroid Problems: A personal history of thyroid disease, including goiter, raises risk.
- Previous Thyroid Surgery: Surgical removal of part or all of the thyroid increases risk.
- Previous Radiation Treatment: Radiation to the thyroid, neck, or chest can impair thyroid function.
- Family History: A family history of thyroid disease increases susceptibility.
- Pregnancy: Pregnant women are at increased risk.
- Recent Childbirth: Women who have given birth within the past six months are at higher risk.
Other major risk factors include:
- Autoimmune Diseases and Genetic Disorders: Examples of genetic disorders include Turner syndrome and Down syndrome.
- Drinking and Smoking: Alcohol may reduce iodine absorption, impair liver function involved in thyroid regulation, and contribute to thyroid inflammation. Smoking affects thyroid hormone levels in complex and sometimes opposing ways and may alter TSH levels.
- COVID-19 Vaccination: A 2025 study comparing more than 1.1 million vaccinated people with an equal number of unvaccinated people found an association between vaccination and increased risk of hypothyroidism.
- PFAS Exposure: Higher levels of certain perfluoroalkyl and polyfluoroalkyl substances (PFAS), often called “forever chemicals,” have been associated with changes in thyroid hormone levels and increased risk of subclinical hypothyroidism.
- Thyroid-Stimulating Hormone Test: Measures TSH levels in the blood. A high level usually indicates that the thyroid is not producing enough hormone.
- Thyroxine (T4) Test: Measures the level of thyroxine in the blood to assess thyroid function.
- Thyroid Antibody Test: Detects antibodies that may signal autoimmune conditions linked to hypothyroidism.
- Complete Blood Count: Measures levels of red blood cells, white blood cells, and platelets.
- Imaging Tests: May include a thyroid scan, ultrasound, or a radioactive iodine uptake test, which measures how much radioactive iodine the thyroid absorbs from the blood after a small oral dose.
Currently, guidelines for hypothyroidism screening vary, but testing is recommended for certain groups—such as newborns and older adults at risk.
Thyroid Hormone Replacement Therapy
Treatment typically involves oral thyroid hormone medication, including:
- Levothyroxine (Synthetic T4): The preferred treatment for hypothyroidism. The dose is tailored to age, body size, overall health, and absorption. The goal is to bring TSH into the mid-normal range and maintain it there. Overtreatment is avoided because excessive thyroid hormone can strain the heart and increase osteoporosis risk.
- Liothyronine (Synthetic T3): Not recommended for long-term therapy because it can cause rapid hormone fluctuations and increase cardiovascular risk. Liothyronine is mainly used for rapid correction in myxedema crisis.
- Combination T3 and T4 Therapy: Oral combination treatments may cause fluctuations in T3 levels, though the peaks are lower than with synthetic T3 alone because smaller amounts are used. By contrast, treatment with synthetic T4 alone produces a gradual rise in T3 levels that remain stable when dosing is appropriate.
- Desiccated Animal Thyroid Products: These dried animal-derived products contain variable amounts of T3 and T4 and are generally not recommended unless a patient is already stable on them with normal TSH levels. Desiccated thyroid extract was the first treatment for hypothyroidism, used before synthetic levothyroxine was developed. However, because they were introduced before modern drug approval standards, they have not undergone the same regulatory process. Many patients in the United States continue to prefer them as their treatment of choice. In August 2025, the Food and Drug Administration stated that it was committed to seeking the first-ever approval of desiccated thyroid extract, pending results from ongoing clinical trials.
It’s generally recommended to wait at least four hours between taking thyroid hormones and other medications, supplements, or foods that may interfere with absorption, including certain antacids, calcium, iron, soy, and high-fiber foods.
Medicinal Herbs
A 2024 systematic review of five studies found that herbal medicines increased T4 and T3 levels and lowered TSH levels compared with placebos. A 2025 review concluded that herbal therapies show potential for treating hypothyroidism, but large-scale randomized controlled trials are needed to confirm their safety, effectiveness, and possible interactions with conventional treatment.
Acupuncture
In addition to relieving pain, acupuncture may help regulate immune function and support immune balance. A 2018 review found that acupuncture, used alone or alongside other therapies, may help reduce symptoms and improve biomarkers in patients with thyroid disorders, including hypothyroidism.
1. Diet
Diet can support thyroid hormone production and function.
- Iodine-Rich Foods: Iodized salt, seaweed, seafood, saltwater fish, nori, and sea salt provide iodine needed for hormone production. However, since excessive iodine intake can lead to thyroid disorders, it is important to consult your health care provider before increasing intake.
- Selenium-Rich Foods: Selenium is vital for proper thyroid hormone function and metabolism. Brazil nuts, seafood, meat, poultry, dairy products, whole grains, garlic, and onions support thyroid hormone activation and help protect thyroid tissue.
Foods to limit:
- Soy: Tofu and edamame (immature soybeans) may reduce absorption of thyroid medication.
- Raw Cruciferous Vegetables in Large Amounts: Foods such as broccoli and cabbage can interfere with thyroid hormone production, particularly when iodine intake is low.
- Highly Processed Foods: Foods high in added sugars, salt, and unhealthy fats may contribute to weight gain, inflammation, elevated blood pressure, and impaired thyroid hormone conversion.
- Gluten: May worsen autoimmune thyroid conditions in people with gluten sensitivity or celiac disease.
- Excess Fiber: Large amounts may reduce absorption of thyroid medication, though moderate fiber intake remains beneficial.
- Coffee: Caffeine may limit the absorption of thyroid hormone replacement if taken too close to medication time.
Gut health also plays an important role in thyroid health. An imbalance in gut bacteria (dysbiosis) has been linked to thyroid dysfunction, while a healthy microbiota may help prevent and manage thyroid disorders. Probiotics can help promote beneficial gut bacteria, enhance mineral absorption important for thyroid activity, and help support thyroid hormone balance.
2. Supplements
Inform your doctor about any supplements you are taking or considering to avoid interactions with thyroid medications.
- Iodine: Supplementation may benefit people with iodine deficiency. However, excess iodine can worsen autoimmune thyroid conditions, including Hashimoto’s thyroiditis.
- Selenium: A 2019 meta-analysis found that people with hypothyroidism often have lower selenium levels. Supplementation may also help normalize TSH levels in selenium-deficient people with subclinical hypothyroidism.
- Zinc: Zinc supports thyroid hormone production, and thyroid hormones support zinc absorption. A deficiency in one may affect the other. While research shows that zinc supplementation can improve thyroid function, excessive zinc intake may disrupt immune balance and increase autoimmune thyroid risk.
3. Long-Term Exercise Therapy
A 2025 meta-analysis found that long-term exercise interventions (at least eight weeks, three days a week) alongside standard treatment can improve thyroid function in hypothyroid adults by lowering TSH and increasing T4. The exercise interventions used in the studies include aerobic exercises, resistance training, endurance training, and gentle exercises such as walking and swimming.
4. Yoga
A 2021 study of 38 women with hypothyroidism and mild to moderate depression found that a three-month yoga program alongside medication improved symptoms. Participants experienced reductions in depression, TSH levels, fatigue, anxiety, and stress, along with improved high-density lipoprotein (HDL) cholesterol levels.
5. Aromatherapy
A 2019 study found that inhaling a blend of peppermint, black pepper, clove, grapefruit, and bergamot essential oils may reduce fatigue in women with hypothyroidism, particularly global and affective fatigue.
6. Earthing
Earthing, also called grounding, is a therapeutic practice that reconnects the body with the earth’s surface electrons, which are thought to help neutralize harmful free radicals. This process may reduce inflammation, support the immune system, and provide the body with natural antioxidants. Earthing can be practiced outdoors by standing barefoot on grass or indoors using a grounding system while sleeping, relaxing, or working.
- Anemia: Thyroid hormones help deliver oxygen to tissues and stimulate a hormone called erythropoietin, which promotes red blood cell production. When thyroid hormones are low, red blood cell production slows, leading to anemia.
- Infertility and Birth Defects: Low thyroid hormone levels can disrupt reproductive hormones and impair early fetal growth and brain development, increasing the risk of infertility, miscarriage, and birth defects.
- Increased Infection Risk: Low thyroid hormone levels can weaken the immune response, making it harder to fight infections such as pneumonia.
- Heart Disease: Low thyroid hormone levels can raise LDL cholesterol, contributing to atherosclerosis and heart disease.
- Heart Failure: Slowed heart rate and weakened pumping ability can reduce blood flow and increase the risk of heart failure.
- Peripheral Neuropathy: Nerve damage may cause pain, burning, tingling, numbness, muscle weakness, or loss of muscle control.