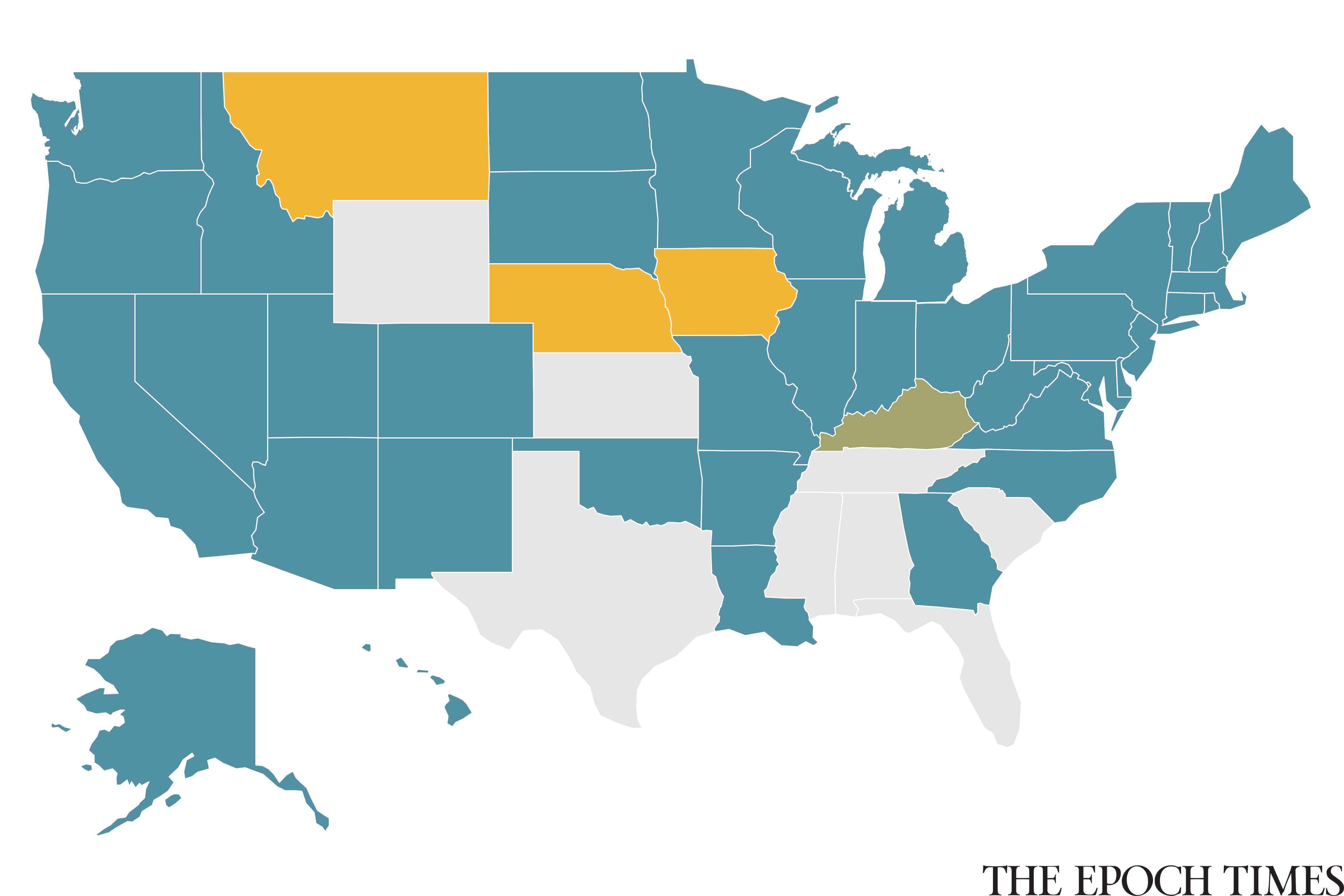
Federal law will require that adults enrolled in the Medicaid expansion meet new work requirements starting on Jan. 1, 2027, though several states are implementing them sooner.
Nebraska started its program on May 1. Montana and Iowa plan to start in July and December, respectively.
The new rule will require Medicaid expansion recipients to complete 80 hours of work or approved activities each month.
Qualifying activities include community engagement, job training programs, or being at least a half-time student.
Americans can qualify for Medicaid—a joint federal and state program that helps cover medical costs—based on income, household size, disability, family status, and other factors. Requirements and benefits can vary by state.
In 41 states that have expanded Medicaid coverage, people can qualify based on income alone.
The Congressional Budget Office estimated about 18.5 million people would be subject to the requirement each year starting in 2027.
Here is what we know about who is affected and how the states will implement Medicaid work requirements.
Who Is Affected
Medicaid expansion typically covers adults with incomes between 100 percent and 138 percent of the federal poverty level.
As of 2026, this threshold translates to nearly $16,000 to $22,000 annually for an individual, or $33,000 to $45,000 for a family of four.
Exemptions exist for certain groups, such as those with young children. However, parents with children aged 14 or older are generally not exempt.
“This means that many poor parents with teenagers must meet work requirements or be exempt,” said Tricia Brooks, research professor at Georgetown University’s Center for Children and Families, in an April 30 KFF event.
KFF is a leading U.S. health policy research organization.
There is also an exemption for people considered “medically frail.” But states are struggling to define exactly who qualifies for this without clearer federal guidance, said Kate McEvoy of the National Association of Medicaid Directors.
“Although states face a great deal of uncertainty over how to define and verify medical frailty because [Centers for Medicare and Medicaid Services] has not yet issued formal guidance, they are nevertheless moving forward with putting structures in place,” said McEvoy.
The Medicaid expansion added nearly 20 million to the 45 million traditional Medicaid enrollees, as of June 2025.
Among the expansion population, roughly 21 percent reported not meeting work requirements and may not qualify for an exemption.
Under the new policy, states would lose federal Medicaid funding for able-bodied adults who fail to meet the requirement.
Federal Medicaid coverage is projected to decrease by 5.2 million adults in 2034, according to the Congressional Budget Office.
Medicaid spending is expected to be cut by more than $344 billion over a decade.
Implementation and Verification
Most states are planning to adopt optional hardship exceptions to work requirements, including individuals receiving care in a hospital or nursing facility, traveling for medical treatment, living in an emergency or disaster county, or living in a high-unemployment county.
Medicaid will generally no longer be available for refugees, asylees, victims of human trafficking, and humanitarian parolees starting on Oct. 1, according to State Health and Value Strategies.
Only lawful permanent residents, certain Cuban and Haitian immigrants, and people from Micronesia, Palau, or the Marshall Islands will remain eligible.
In many states, lawfully present children or pregnant immigrants can also enroll with no waiting period.
Federal law requires states to check enrollee compliance with Medicaid work requirements every six months. Indiana and New Hampshire require quarterly compliance checks.
To reduce the paperwork burden on individuals, states are trying to use automated data matching.
By linking Medicaid systems with other programs like food stamps or private payroll services like Automatic Data Processing, states can sometimes verify a person’s work status or income without requiring them to submit manual documents.
Lawrence Wilson contributed to this report.