Robin Wayman had never heard of glossopharyngeal neuralgia before being diagnosed with the condition in 2025.
The rare illness causes excruciating pain in the ears, jaw, tongue, and tonsils.
Wayman, 64, found a neurosurgeon in Atlanta who could treat the problem. She traveled from her home in Seymour, Tennessee, for pre-surgery tests and an appointment with the hospital’s business office.
A representative presented Wayman with a form stating the amount to be paid by her insurer, about $16,000, and the amount she would owe, about $4,000. She signed the statement and made an initial payment of more than $1,000.
A few weeks later, Wayman underwent a successful procedure. While recovering at home, she continued making payments to the hospital.
Months went by.
Then Wayman received another bill—for $80,000.
Thinking it was a mistake, she called the hospital. The billing representative said the charge was accurate.
“Why didn’t I know this up front?” she said. “I would have searched for care somewhere else.”
The agent’s reply dumbfounded Wayman.
“He said, ‘I’m sure you would have, ma‘am, but you owe it,’” she said.

Robin Wayman appears in Seymour, Tenn., on Feb. 14, 2026. (Courtesy of Robin Wayman)
“I was sick,” she said. “I could not sleep. I didn’t know what I was going to do.”
An overwhelming majority of Americans have health insurance. Yet many face mystifyingly high medical charges, often revealed only after receiving treatment.
For them, the cost of health care is more than the tens of thousands spent on insurance premiums and medical bills.
It includes countless hours seeking answers from providers and insurers who, they say, sometimes seem intent on concealing the cost rather than revealing it.
For many patients, billing departments add another layer of stress to medical treatment. Some report worrying less about the prospect of surgery than about how to pay for it or whether to have it at all.
Some patients feel frustrated, others angry or victimized. Many find themselves asking some version of a familiar question: Why won’t they just tell me how much this is going to cost?
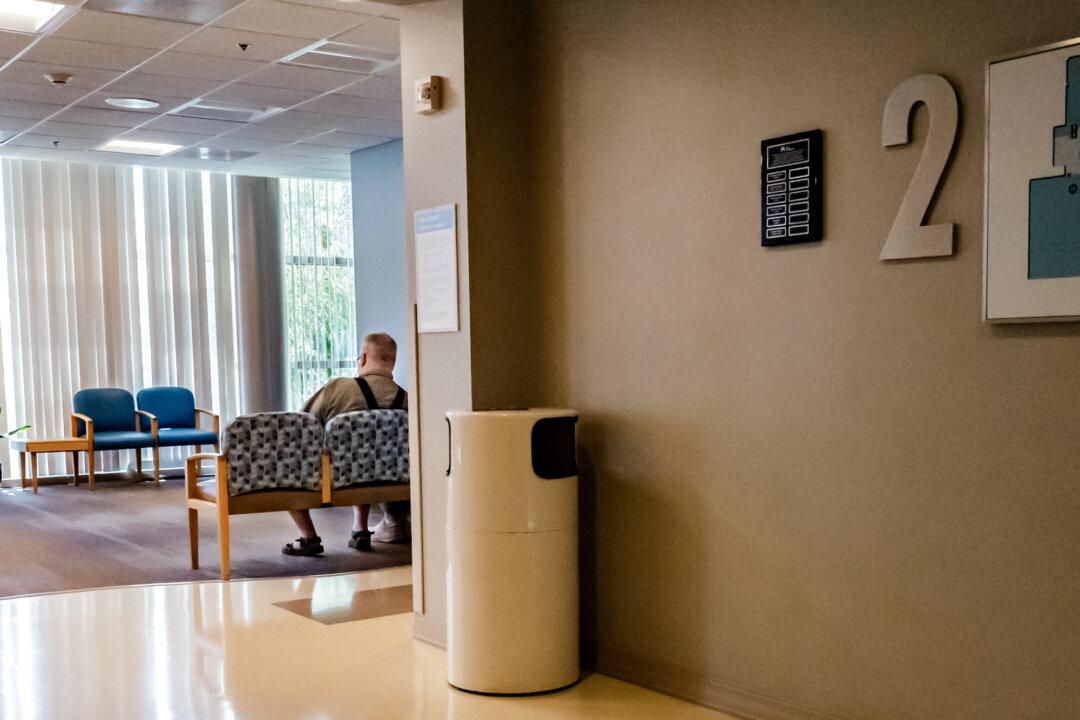
A man waits in a hospital in Irvine, Calif., on July 8, 2025. The overwhelming majority of Americans have health insurance. Yet many face mystifyingly high medical charges, often revealed only after receiving treatment. (John Fredricks/The Epoch Times)
‘Nobody Explains It’
Mark Thompson, 55, of Albuquerque, New Mexico, went to a hospital outpatient department for routine hernia surgery in 2024.
Medicare allows about $2,900 for a straightforward hernia repair if performed at an ambulatory surgery center, or about $5,700 at a hospital outpatient department.

Mark Thompson is shown in Columbus, Ga., in October 2025. (Courtesy of Hazel Shirley)
This hospital charged Thompson $93,826.
“I don’t know where all the money goes,” Thompson told The Epoch Times. “Nobody understands it, nobody explains it, and the people they have answering the phones aren’t much help.”
Dr. Marty Makary, commissioner of the Food and Drug Administration, seems to agree.
“Hospital charges are notoriously inflated—and hard to pin to any actual cost,” Makary wrote in his 2019 book “The Price We Pay: What Broke American Health Care—and How to Fix It.”
Makary said hospital CEOs regularly told him that they didn’t expect anyone to pay the excessive prices, that they were merely a starting point for negotiations with insurance companies.
But people do pay them.

Health care workers walk down a hospital hallway, in this file photo. (Alamy/PA)
Going Without Medication
Many patients have a choice of providers for treating common illnesses, but not everyone.
Kevin Baker, 23, of Eugene, Oregon, takes medication to control Crohn’s disease. The prescription costs more than $6,500 per month. The medication is under patent, so it’s available from only one manufacturer.
Baker has health insurance, but his insurer refused to pay for the drug. And although the manufacturer provides financial assistance to some patients, the amount changes from year to year.
“It runs out eventually,” Baker told The Epoch Times. “And they don’t always tell you when.”
That has left him with unexpected bills up to $2,000.
“There have been times I have to go without medication that I need just to live day to day,” he said.
“I just have a feeling these people in the boardrooms know that I need this, so they can charge me whatever they want.”

Kevin Baker in Leavenworth, Wash., in January 2024. Baker takes medication that costs more than $6,500 per month to control Crohn’s disease. (Courtesy of Lauren Baker)
‘No Warning’
The No Surprises Act of 2021 was intended to keep patients from receiving unexpected medical bills, especially from out-of-network providers.
Yet those bills continue to be issued.
Patricia Martin is shown in Brunswick, Ohio, in December 2025. (Courtesy of Danielle Martin)
Patricia Martin, 67, of Brunswick, Ohio, noticed an extra charge of $368 on her bill after a follow-up appointment for osteoporosis.
“I thought I was being charged twice because it was almost the same amount as what the nurse practitioner charged me,” Martin told The Epoch Times.
But it wasn’t a duplicate. It was a facility fee, which many hospitals charge over and above fees for medical treatment. Hospitals can generally add these charges at any facility they operate—whether attached to a hospital or not.
Martin saw a nurse practitioner at a freestanding professional office.
“I was just in shock,” she said.
This was the first time she’d been charged a facility fee when seeing that particular provider.
“They’re all of a sudden putting this fee on, and they give no warning,” Martin said.

A medical staff member walks inside Lenox Health Greenwich Village Hospital in New York City on Nov. 2, 2020. (Chung I Ho/The Epoch Times)
‘Really Frustrating’
Many patients don’t ask about the fees before treatment. Those who do may be no better informed.
Thompson requested a statement of cost before his hernia surgery, but had trouble getting one.
“My insurance company asked them multiple times what my part would be, so my family and I could budget,” Thompson said.
He got no answer until the day before the surgery, and then only after threatening to cancel the procedure unless a price was quoted.
The estimate stated that the insurer was responsible for $90,238. That left $3,588 for Thompson to pay.
He paid the full amount on the day of the surgery, which was completed without complications.
But the next week, more bills arrived. There were bills from the anesthesiologist, the surgeon, a physician assistant, and others he couldn’t identify.
“They were fairly small, a couple hundred dollars each, so I just paid them,” Thompson said.
But when the bills kept coming, he started asking questions.

Medical bills, in Temple Hills, Md., on June 26, 2023. (Jacquelyn Martin/File/AP Photo)
Thompson spent hours on the phone trying to learn what the charges were for and why he hadn’t been informed of them beforehand. No one seemed able to provide answers.
Then the hospital sent another bill for $1,779 on top of what he’d already paid.
“It was really frustrating, really time consuming, really expensive, and it just didn’t make any sense,” Thompson said. “I’ve never been around an industry where you don’t give people your prices, and can’t explain them even after the fact.”
‘It’s Predatory’
Provider discounts can be equally difficult to understand.
Elizabeth M., 28, of Cincinnati, discovered as much after being diagnosed with non-radiographic ankylosing spondylitis at age 23. She asked to be identified by first name only.
Her condition improved greatly with medication, but the medication cost more than $5,700 per month. Her insurance paid most of that, but the copay was still more than she could afford.
Fortunately, the manufacturer offered a copay card. She could present it at the pharmacy to receive a credit equal to her copayment amount.
“But I had no visibility into it,” Elizabeth said, meaning that she never knew the balance remaining on the copay card.
Even so, the system worked until her insurer stopped allowing refills for an 84-day supply. Elizabeth then had to refill the medication every 24 days.
That increased the number of copayments, leaving Elizabeth with a larger share of the total cost. By April of that year, she had exhausted her copay card without realizing it.

A pharmacy manager works in the new Amazon pharmacy in Corona, Calif., on May 29, 2024. (Terry Pierson/The Orange County Register via AP)
The insurer refused to return to an 84-day supply, and the manufacturer wouldn’t add more funding to the copay card. Mercifully, her physician was able to provide free samples of the drug.
“Fortunately I am able to be on the phone with the insurance company, the drug manufacturer, my doctor’s office, and the pharmacy,” Elizabeth said, comparing it to having a part-time job.
Yet she said she fears for critically ill patients who may lack the energy or ability to deal with the intricate pricing, discount, and payment arrangements used by providers and insurers.
“I think it’s predatory,” she said.
Threatened With Collections
Patients wonder about the seemingly arbitrary prices charged for medical treatment. They can be equally mystified when those charges suddenly vanish.
Wayman spent months fretting about her $80,000 medical debt. Her son enlisted a patient advocacy group to negotiate the charges, but the hospital refused to budge.
“It was hanging over my head all summer,” she said. “I could never rest easy.”
That fall, a letter arrived in the mail.
“I got notification that they just marked my bill off,” she said.
After months of insisting that she owed $80,000, saying she didn’t qualify for financial aid, and repeatedly refusing to lower the bill, the hospital dismissed the debt without explanation.
Thompson’s original charge of more than $93,000 was discounted by more than $50,000 by the hospital. The insurer paid $12,523.
After being threatened with collections, Thompson agreed to negotiate his remaining balance with the hospital.
“You kind of give in,” he said. “You don’t really have a choice.”
When he pulled out his credit card and asked for a deal, a hospital representative immediately agreed to accept less than half of the remaining balance.
“They quickly settled,” Thompson said. “It’s really funny.”

A man walks through a hospital in Irvine, Calif., on Oct. 11, 2016. (John Fredricks/The Epoch Times)
‘Existential Dread’
Thanks to the tens of thousands of dollars spent on insurance premiums and out-of-pocket payments, occasional provider discounts, intercession by patient advocates, and countless hours on the phone, these patients have been able to pay their medical bills so far.
Each of them seems happy and fully engaged in life.
Yet a nagging question lingers in their minds: What if I can’t keep paying for this?
Emily Grant, 33, of Fort Worth, Texas, recalls the day that she realized the financial burden of her illness.
Grant has cystic fibrosis and a related case of diabetes. As a teenager, she was already taking several expensive medications.
Health insurance premiums were rising for the school district where her father worked, and Grant knew that her illness was a big part of the cost.
“The school district tried to fire my dad in order to reduce health care costs,” she told The Epoch Times. “Obviously, that was all me.”
Since then, the Affordable Care Act has prohibited insurers from raising premiums based on the health of an individual enrollee.
Now married with three children, Grant requires 25 prescription pills, eight nebulizer breathing treatments, and up to six insulin shots each day to remain healthy.

Emily and Eric Grant pose at the Kimbell Art Museum in Fort Worth, Texas, on Oct. 16, 2025. Emily, who has cystic fibrosis and related diabetes, said she has faced the financial burden of her illness since her teenage years. (Courtesy of Danyelle Snead)
Her insurance premiums and out-of-pocket maximum total $26,000 a year, a number that’s never far from her mind.
“I am constantly working out ways that I can save money, that I can put away for a rainy day in case something happens and we need to pay more,” she said.
Elizabeth M. describes that feeling as “a little bit of existential dread.”
Some patients are reluctant to seek medical treatment for fear of being ambushed by unreasonable charges.
“I try to avoid going to the doctor because of that,” Martin said.
“I’m never having any kind of surgery ever again,” Wayman said. “Unless it’s to save my life.”